Editor’s note: A previous version of this blog post had an error in the HLA table, which has been corrected in this version.
By Janie Shelton, Ph.D., and Daniella Coker, MPH*
As part of 23andMe’s ongoing study into COVID-19, our scientists have recently looked at how people react differently to different vaccines, noting that those who previously had COVID-19, as well as women and younger people reacted the strongest to the vaccine.
Following up on that data, we also wanted to better understand whether genetics could help explain those differences and whether that could help us better understand the virus. We found that some variants in a complex of genes involved in immune response are associated with being more likely to have a strong reaction to the vaccine and some make it less likely.
Participating in COVID-19 Research
Before we go into details it’s important to note that this kind of study is possible because millions of individuals have already been vaccinated. Among them are a large number of 23andMe customers who have consented to participate in research. That has allowed our scientists to quickly explore how genetics plays a role in both the susceptibility and severity of COVID-19. We’ve also looked at other aspects of the pandemic like its impact on sleep, physical activity, and how it has hit some communities harder than others. In this latest study, we looked at the factors associated with “reactogenicity”, or how noticeable a person’s response was to the vaccine. Some reported feeling nothing at all while others reported feeling very ill. This gave our scientists the data needed to study whether genetics could explain those differences.
To do that we conducted a genome-wide association study looking at these different responses to the vaccine between those who described feeling “Not at all sick” to those who felt “Extremely sick.”
Genetic Associations
We found a strong association between variations in the HLA genes — the human leukocyte antigen complex which is involved in regulating immune response. These genes encode for a number of proteins that make up the major-histocompatibility complex, which is on the frontline of your immune system’s infection recognition system. These results show that variations in the HLA complex are related to the degree to which one feels ill after vaccination.
First, it’s helpful to understand a bit about how vaccines work. These vaccines teach your immune system to recognize and respond to the virus that causes COVID-19. The mRNA vaccines (e.g. Pfizer/BioNTech & Moderna) introduce genetic instructions to make a harmless protein that is unique to the virus. The other most common vaccine in circulation is the Johnson & Johnson/Jansen vaccine, which uses a viral vector encoding the spike protein. In all three of these vaccines, your immune system develops a response to the spike protein of SARS-CoV-2, so your immune system can recognize the virus faster if you become exposed and eliminate it before you become severely ill.
Immune Response
Given how the vaccines work, why would we expect the HLA to be involved? The primary function of HLA molecules is to present foreign antigens on the cell surface in order to elicit an immune response. As such, the HLA plays a key role in presenting the proteins derived from the vaccine to the immune system.
But why do some people feel very sick from their COVID-19 vaccine, and others don’t feel sick at all?
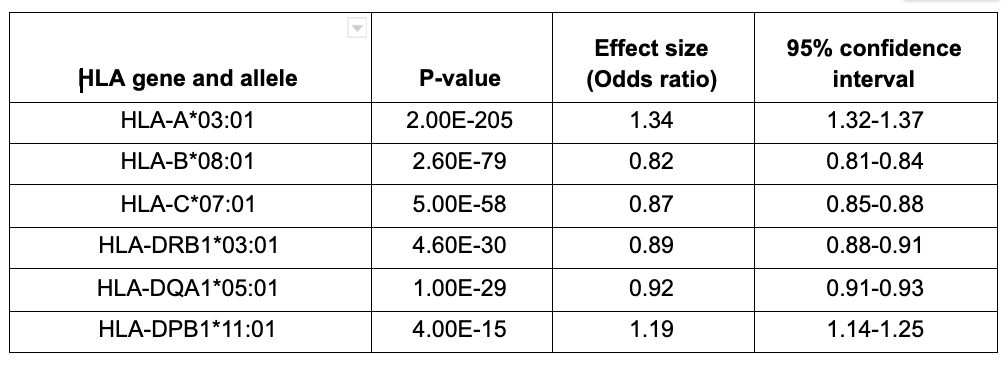
Our findings suggest that prior history of COVID-19, younger age, female sex, and the type of HLA alleles you carry are strong predictors. Note that in the below table effect sizes below 1.0 decrease the likelihood of a reaction to the vaccine and the ones above 1.0 increase the likelihood (all reported effect sizes are statistically significant after correction for multiple tests).
Long-haulers
Other studies have also found variation among populations for other alleles within the HLA that are associated with the severity of COVID-19. So for example, a recent study by researchers at the Translational and Clinical Research Institute within Newcastle University found that an allele protective against severe COVID-19 symptoms in the HLA gene, at HLA-DRB1*04:01, was found at much higher frequency in people of Northwestern European ancestry. (Other studies have also found a genetic link to susceptibility to pneumonia, also linked to genes associated with immune response.)
23andMe’s data on genetic associations related to different reactions to the vaccine offers other clues about the complexity of COVID-19. It is part of our on-going work to better understand the virus and the best approaches to fight it. Along with the workaround how genetic differences in immune response and blood type may play a role, our researchers are studying the long-term effects of the virus. We hope to look at so-called COVID-19 long-haulers to determine whether genetics can also explain why some individuals suffer health effects from the virus for weeks, months, and longer.
For more, you can go to our COVID-19 Information Center here.
*The 23andMe COVID-19 research team includes: Adam Auton, Adrian Chubb, Alison Fitch, Alison Kung, Amanda Altman, Andy Kill, Anjali Shastri, Antony Symons, Catherine Weldon, Chelsea Ye, Jason Tan, Jeff Pollard, Jey McCreight, Jess Bielenberg, John Matthews, Johnny Lee, Lindsey Tran, Maya Lowe, Michelle Agee, Monica Royce, Nate Tang, Pooja Gandhi, Raffaello d’Amore, Ruth Tennen, Scott Dvorak, Scott Hadly, Stella Aslibekyan, Sungmin Park, Taylor Morrow, Teresa Filshtein Sonmez, Trung Le, and Yiwen Zheng.




