An international team of scientists has identified two genetic variants that influence the odds of a mother having natural fraternal, non-identical, twins.

Hamdi Mbarek
Fertility
The findings also offer more insight into female fertility and ovarian function as one of the variants is near a gene called FSHB that plays a role in the onset of puberty in girls, age of menopause, and risk for polycystic ovary syndrome (PCOS), a leading cause of infertility.
The findings, published in The American Journal of Human Genetics could have important clinical value for treatment of female infertility, including hormonal stimulation for ovarian production, which is commonly used for In Vitro Fertilization (IVF). They might also help clinicians identify women who are more likely to have twins or triplets while undergoing IVF.
The authors of the paper said the study will have “important implications for human fertility, including improved outcome prediction and novel avenues of fertility treatment.”
Maternal Genetics and Twins
Although it has long been established that there was a maternal genetic component to non-identical twinning, this is the first time that scientists have identified the possible genes involved.
About 1-to-4 percent of babies born is a fraternal, or dizygotic, twin. However, a mother with one of the variants identified in this study increases her odds of naturally having multiples by 9-to-18 percent, according to the study. The increase goes up to 27 percent if she has one of each variants.
This type of “twinning” occurs when more than one egg is released in a woman’s cycle and fertilized. Identical, or monozygotic, twins are much rarer, accounting for just a quarter of all twin births. Research has not shown that having identical twins is influenced by genetics.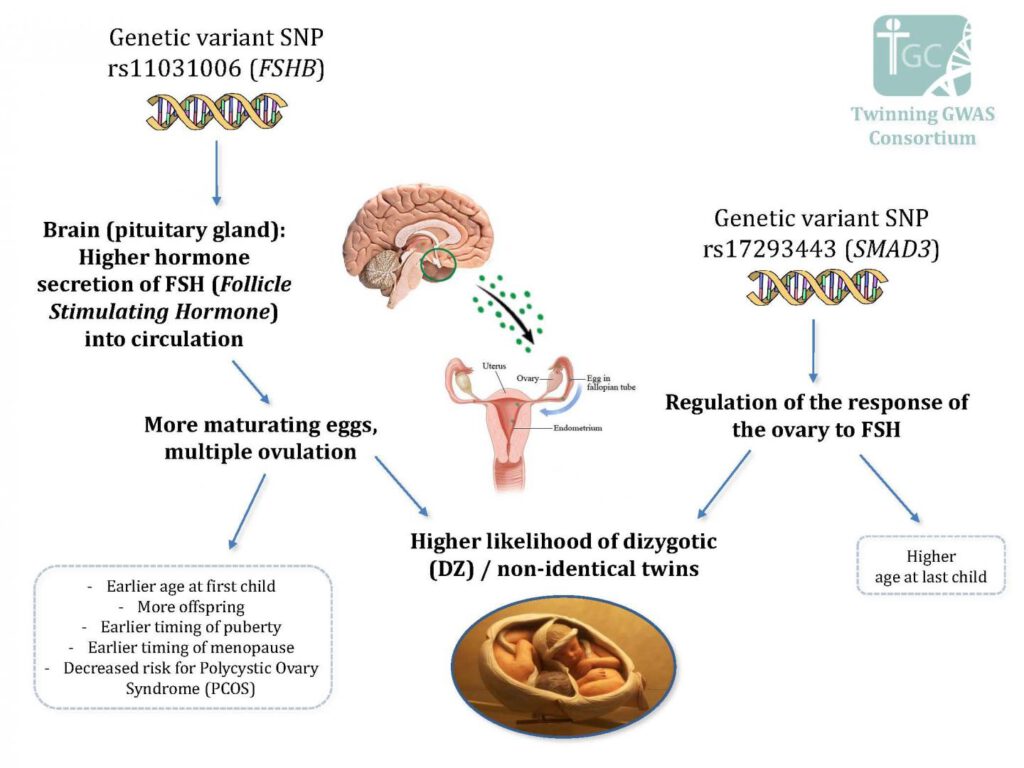
The Role of Hormones
Hamdi Mbarek and Dorret Boomsma from the Vrije Universiteit Amsterdam lead the international team. The researchers identified one genetic variant located near the FSHB gene that encodes a portion of follicle-stimulating hormone (FSH). The FSH hormone is important for the menstrual cycle and egg production in women. This variant was also associated with higher FSH levels. Higher FSH levels is associated with earlier age at menarche and menopause, earlier age at first child and last child, increased number of children, and decreased risk for PCOS.
The second genetic variant identified in this study is located in a gene called SMAD3. The authors speculate SMAD3 may influence how the ovaries respond to the FSH hormone.
For their research the scientists conducted a genome-wide association study using data from 1,980 mothers of natural fraternal twins. They used additional data from about 13,000 mothers of non-twins from cohorts in the United States, Australia and the Netherlands. Most of the data was from a large Icelandic cohort assembled by the company DeCODE.
The findings were also replicated using data from another 300,000 cases and controls from DeCODE.
Data from 23andMe’s study on the onset of puberty in women was used in this research. The study also included data from another study on the genetic associations with PCOS. All together those studies included data from more than 160,000 female 23andMe customers who consented to research.



