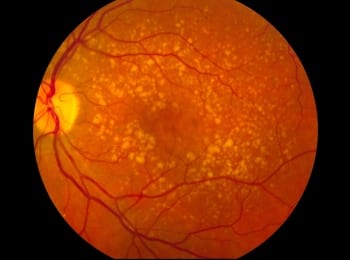
A new treatment for one type of age-related macular degeneration that is currently in clinical trials may have an unintended consequence: it could cause another form of the disease.
Age-related macular degeneration (AMD) is the most common cause of irreversible vision loss in the western world among people over 60. The two forms of the disease — wet and dry —both cause vision loss by destroying cells in the central portion of the retina.
In the last few years, progress in understanding AMD has been made thanks in part to the discovery of several genetic variants linked to both forms of the disease. Yesterday a report published online in the New England Journal of Medicine described yet another AMD genetic association, this time specific for the dry form of the disease.
The variant is in the gene for toll-like receptor 3 (TLR3), a protein that helps the immune system fight off viruses.
“What TLR3 does in the case of infection is sacrifice an infected cell to protect the neighborhood,” said the study’s senior author Kang Zhang in a statement.
Lab tests in human eye cells and genetically engineered mice found that the T version of the SNP decreases TLR3’s cell killing potential by reducing its activation in response to viral cues. Studies of patients and controls found that version of the SNP also decreases the risk of developing dry AMD.
“This discovery has significant implications for diagnosing the dry form of AMD, which is the most prevalent form. It also allows us to develop new drugs to the treat the dry form of AMD, for which there is currently no treatment,” Zhang said.
Jayakrishna Ambati, another author of the study, plans to start clinical trials testing the effectiveness of TLR3 inhibitors in patients at risk for developing dry AMD next year.
The discovery of the role of TLR3 activation in dry AMD may have come just in time. Several drugs for the treatment of wet AMD currently in clinical trials may actually trigger the protein, thus treating one form of the disease while causing the other.
The new treatments for wet AMD are based on a general method called RNA interference (RNAi) that uses short RNA molecules to interrupt genes. In wet AMD, the goal is to disrupt genes involved in the aberrant blood vessel growth seen in the eyes of patients.
Research from Ambati’s lab published earlier this year, however, found that RNAi treatments (regardless of their target), activate TLR3. The immune protein confuses the RNA molecules with the genetic material of viruses, its sworn enemies.
People with the another variant that is protective against AMD might still be good candidates for RNAi treatments for wet AMD. Their TLR3 proteins are naturally less reactive. But for the 43% of people of European ancestry with two copies of the more deliterious variant, these treatments could do more harm than good.
“Ironically, in some individuals, using RNAi to cure wet AMD might actually increase the risk for blindness from dry AMD,” Zhang said.