This post has been updated. It was originally published on May 26, 2023.
Can learning about your Irish ancestry also give you a chance to prevent serious health consequences? When it comes to the “Celtic Curse” the answer is yes.
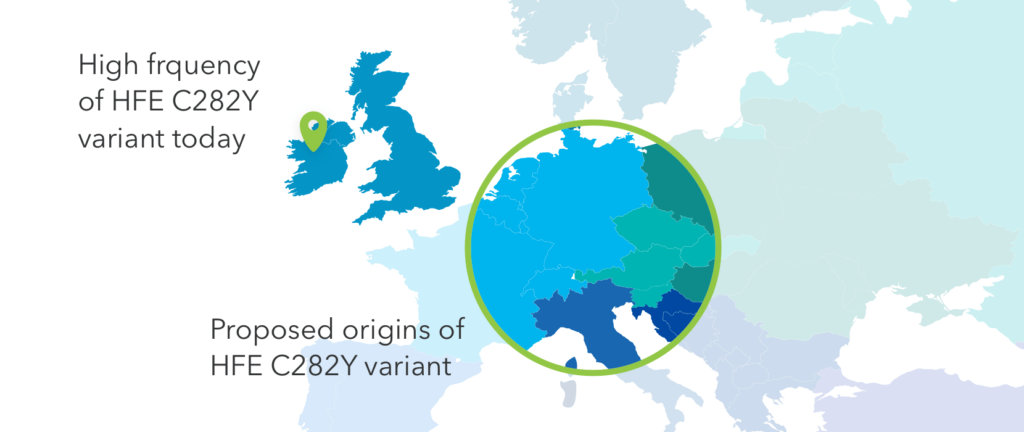
Thousands of years ago people from central Europe came to the British Isles. It’s thought that some of them carried slight changes in their genomes that may have protected them from iron-deficient diets. These small changes—two genetic variants in the HFE gene—spread and became especially common in Ireland.
Today, however, those two genetic variants can turn deadly, as they’re linked to a genetic condition called hereditary hemochromatosis. Dubbed the “Celtic Curse,” because it tends to affect people with roots in Ireland and the UK, hereditary hemochromatosis can lead to toxic iron accumulation in a person’s organs. The condition is highly treatable when caught early, but many people go undiagnosed.
A Common Genetic Disease You Never Heard Of
Hereditary hemochromatosis often goes undetected for years, decades even. By then, the disease may have already done its damage to organs. Even though it is one of the most common genetic diseases, many people have never heard of it.
Casey Hill certainly never had.
“I didn’t know at the time exactly what it meant or how serious it could be.”

No This is Serious
When the 31-year-old Head of Growth for a video messaging app used 23andMe, it was to learn about his ethnic origins, which are primarily British and Irish.
“I originally got 23andMe to learn more about my ancestry,” Casey said. “But then it turned into much more.”
After perusing what 23andMe had to say about his ancestry, Casey viewed the health tutorials and opened up his genetic health risk reports. A few things drew his attention. First, he had a single genetic variant associated with a slightly increased risk for celiac disease* and another for age-related macular degeneration (AMD*). He wasn’t concerned about celiac; the increased risk was minimal. As for his risk for AMD, he took note of it and thought it would be something he should at least be aware of as he got older. Then there was this third thing, a genetic health risk report indicating that he had two copies of genetic variants linked to “Hereditary Hemochromatosis (HFE-Related)*.”
At first, he ignored the details on that report until his wife, who is a doctor, weighed in. She told him this was serious.
“I saw it, didn’t think much of it, but on the advice of my wife, decided to just get (my iron levels) tested,” Casey said.
That’s when he realized just how serious it was. The test showed he already had an iron overload, and should get preventative treatment. His test showed his iron saturation was 91 percent, and he had a ferritin level of more than 600, or about double normal levels.
“If I had waited, I may not have caught it for many more years until it was much worse,” Casey said.
Give Blood
Fortunately, the treatment for hemochromatosis is straightforward and entails periodic phlebotomy. In other words, Casey could lower iron levels by giving blood.
But he was still concerned that he may have already damaged his organs, so he saw a specialist who checked Casey’s liver, kidney function, and heart. Apart from mild toxicity in his liver, his organs looked good, but the specialist was stunned. He told Casey that he wouldn’t generally test for iron overload unless a patient exhibited symptoms. The doctor had no idea that 23andMe even had a report looking at one’s genetic risk for hemochromatosis.
“He thought that was pretty interesting and had never heard of it before,” Casey said.
Left unchecked, hemochromatosis can poison nearly every organ in the body – not just the liver or kidneys, but also the pancreas, heart, and skin. The challenge is catching it early, but the symptoms — such as fatigue and joint pain — are not distinct enough for many people or their doctors to notice. As a result, doctors might not catch the condition until after their patient suffers much more severe consequences, such as heart, liver, or kidney failure.
“23andMe very literally changed my life trajectory by potentially decades,” Casey said.
Understanding your ancestry isn’t just about where you come from, but can also be about taking control of your health.
Find Out More
23andMe Health + Ancestry Service customers can see their Hereditary Hemochromatosis (HFE-Related) Genetic Health Risk report and what it says about their genetic health risk.
Not yet a customer? Find out more about the different services 23andMe offers.
Note:
*The 23andMe PGS test uses qualitative genotyping to detect select clinically relevant variants in the genomic DNA of adults from saliva for the purpose of reporting and interpreting genetic health risks. It is not intended to diagnose any disease. Your ethnicity may affect the relevance of each report and how your genetic health risk results are interpreted. Each genetic health risk report describes if a person has variants associated with a higher risk of developing a disease, but does not describe a person’s overall risk of developing the disease. The test is not intended to tell you anything about your current state of health, or to be used to make medical decisions, including whether or not you should take a medication, how much of a medication you should take, or determine any treatment. For important information and limitations regarding each genetic health risk report, visit https://www.23andme.com/test-info




